
Sale
New In
Pushchairs & Strollers
Car Seats
Nursery
Feeding
Family Hub

Includes Buffet Highchair, Mealtime set, Silicone tray

Includes Clic 2 stroller, Clic stroller bag and rain cover


For the best night’s sleep in every trimester
[TW: This article discusses topics that may be triggering for some readers.]
At the age of 15 and in the midst of life saving chemotherapy, doctors made sweeping statements such as, “Make sure you try for babies in your 20s, as your chances after this are very slim.”
By the age of 34 I’d accepted that surviving Hodgkinson’s Lymphoma was probably enough to be grateful for and despite no signs of early menopause, my chance of becoming a mum was extremely low.

In spite of all this, my only dream really has always been to have a family of my own. At 34 I fell pregnant which filled me with more excitement, anxiety and disbelief than I thought was possible. With health complications from my past plus chronic shingles on my coccyx, fibroids and endometriosis, I was classed as high risk from the beginning. However, despite the hundreds of appointments with consultants and midwives, my pregnancy was absolutely fine. I embraced the extra care and scans and took each step as it came. Morning sickness made some days at work tough, but I felt forever grateful as each scan showed a healthy, growing baby.
My main focus of anxiety throughout pregnancy was the birth, mostly due to being told at 20 weeks that the position of my shingles ruled out any chance of an epidural or spinal block. If a caesarean was needed, then it would be under general anaesthetic.
When I reached 36 weeks my consultant had devised a clear plan of action with me which helped to ease some of my worries. We decided that sweeps would be the first option, induction would be needed if I was to go over 40 weeks, but only on the basis that a C-section could still be elected at any point under general anaesthetic.

At 40 plus 7, three sweeps later, I went in to be induced. Although this wasn’t my ideal plan, I wanted to at least give myself a chance of being awake for my baby’s arrival, rather than heading straight to a GA section. I felt prepared and ready. The pessary was given at 2pm and by 10pm I had contractions and pain which caused the doctor to take a look at me. The decision was made to take me to a delivery suite as I was 3cm dilated, hyper stimulated and in a lot of pain. Contractions came thick and fast; an injection was given to me to try and slow things down and gave me about 20 minutes of relief.
As things progressed, baby’s heart rate started to drop intermittently. The midwife asked me to sit on my left side in the throne position which, with shingles on my coccyx, made things very uncomfortable but totally necessary for baby’s welfare. One consultant visited the room to check on me and I expressed my concern for the baby and explained that I had been reassured if this pain got too much then I could go down for a section. By 3am I was begging to go to theatre, the contractions were not giving me any rest and baby’s heart rate was still all over the place. I quite simply just wanted baby here, no matter whether I was asleep or awake.
By 6:30am, one midwife stated I was 8cm dilated, however, a second assessment from another midwife stated I was only 5cm. I have never felt so disappointed as I did at that moment. My waters were broken at 7am and I begged for a caesarean.
By 11am I was 6cm and totally exhausted and worried, the pain I felt was like nothing I’ve felt before and other than Oramorph (which worried me for baby’s sake) my options were totally out. At 12pm I asked the midwife to check on me because I felt I needed to push. She realised baby was ready to come, but by this point I felt like I had nothing left to give.
At 1:16pm on 26 January our boy arrived. The midwife placed my son on my chest, but I knew in that moment he was not ok. He was blue, and I shouted, “He’s not ok?!” The midwife shouted for the red button to be pressed and suddenly the room was filled with uniforms in seconds.
He was taken from me and placed on a table with wires all around him, surrounded by uniforms so we couldn’t see him. For 15 minutes we waited, the noisy chaotic room felt like it was also silent at the same time. A muffled sound was all I could hear, as though my ears were trying to protect me from what was going on around us.
They worked on our boy and at 1:36pm I finally got to hold him, and he was breathing. The gulp of breath I took when I held him, I will never forget. It felt like I hadn’t breathed for the whole time he was being worked on, nobody spoke, we just waited. For all that time I thought my biggest fears had come true and we had lost him. And for hours later I sat staring at him feeling so blessed that he was here, whilst also battling with why we were the lucky ones when so many don’t get this chance.

Our boy had to be taken to neonatal for just over an hour after our initial snuggles in order to be assessed. His dad went with him while I was able to get stitched and freshened up. Our boy came back, and I sat and fed him his first bottle. What a feeling! He guzzled the whole thing. It was 4pm before we decided to tell anybody that our boy had arrived. Family members had grown increasingly worried because Dan’s updates on our labour had stopped hours before, but I just needed some time to take in what had happened.
I will never forget the faces of the doctors and nurses that came and saved my baby, and their speed to work and bring him back to me. Little did I know this wouldn’t be the last I would see of them.
After announcing the birth of our baby boy to family and friends we were then transferred to the main ward for the evening. We decided to name him Elias – with its link to strength it seemed very fitting. We had visitors and snuggles, and the baby bubble felt so special. I managed to hold my boy as much as I could after losing out on the initial skin to skin when he first arrived.

During the evening, we were told Elias needed some extra heel pricks to check his glucose level due to the way that he had arrived into the world. Sadly, the glucose test showed a low level for him and he would need extra testing throughout the night.
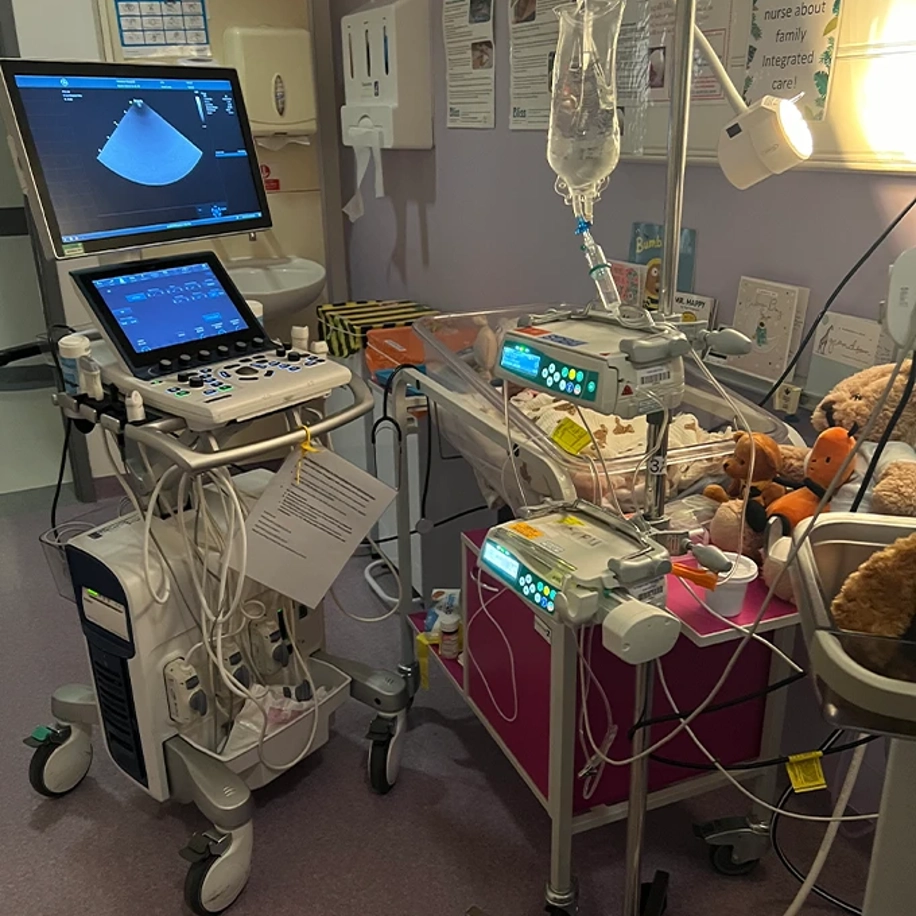
By 9am the next morning, the consultant came into the room to advise that they would need to take Elias away to neonatal as his blood sugars were dangerously low. I couldn’t visit him until lunchtime, once he was set up on the unit. When we visited him, he was positioned in an incubator with a cannula in either hand and suddenly it felt like I couldn’t just scoop my baby up and hold him.
For two whole weeks my baby lay in that incubator with wires and meds; a rollercoaster ride of blood sugar testing every three hours pushed me to my absolute limit of coping. We stayed in hospital in a nearby room on the unit but couldn’t sleep in the same room as our boy, which broke our hearts. I spent my days snatching 20 minutes of sleep here and there trying to avoid him ever being alone.
Some nurses gave me confidence, and some filled me with doubt as numerous errors occurred. Days felt like years and all the time it felt like I was being robbed of those precious days with my baby. Nobody had ever spoken to me about this before birth. I had limited awareness of full-term babies ending up in special care and I most certainly had never heard of congenital hyperinsulinism (CHI). After overcoming what felt like a horrific birth experience, all I dreamt of was taking my baby home, but nobody could promise me when or if that was going to happen.

After two long weeks of restricting milk feeds and increasing glucose on a see-saw method, we finally started to see progress. Elias turned a corner, and sugars started to stabilise so we could finally move to a family room within the special care unit. We had our boy in a room with us, at 13 days old, and it felt like the most terrifying responsibility of my life.
Elias’ start in life was consumed with alarms, tests, medication and a few other more ‘normal’ new mum fears. But the relief of finally bringing home my baby boy outweighed every single worry.
On February 9th, Elias was all ours, we came home with a warning that for at least six months, our lives would be focused on his CHI condition, and we were ready for that. Anything that needed to be done we could do as long as he was ok. His Silver Cross Reef pram was set up and strolling around the park the next day and suddenly it felt like we were going to be ok.

The pregnancy I prayed for, the baby I had dreamed of, and the picture perfect ‘Instagram’ start to motherhood never turned out quite how I had hoped, but here we are now a whole year on with the most amazing, precious little boy who is now fully recovered too. When they say what doesn’t kill you makes you stronger it’s so true. I wouldn’t wish my start to motherhood on anyone, but I hope through my experience I can also help others.
Life is never easy, but it has a funny way of working itself out and guiding us to the things that really matter. My own experience has led me to believe that if I can help even one mum to feel less alienated by birth trauma or time in neonatal, then the pain and lessons learned were all worthwhile.
